Sussex County Parkinson’s Education and Support Group “Vision Statement”
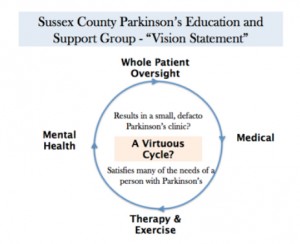
Consistent with the above Vision, our support group is pursuing a number of initiatives
to improve the quality of life of our members with Parkinson?s Disease. The various
initiatives are described below.
Medical
Local medical capability – At the present time (November, 2013) there are no Neurologists on the Delmarva Peninsula who have completed a Movements Disorder Fellowship. There is one such Neurologist in Philadelphia (2 to 3 hours away) who has recently agreed to start a one-day Parkinson?s clinic in our area and if the patient load warrants will expand that to two days a month. This would be a huge improvement over today?s capability which requires our members to make an 8 to 10 hour round-trip to Philadelphia, Baltimore, or Washington, DC to see an expert Parkinson?s doctor. Many of our members, or their caregivers, are not able to make such an arduous trip and therefore are not getting the medical attention they heed. We hope to have this clinic activated within the next few months.
Telemedicine
A number of medical facilities on the Delmarva Peninsula are interested in activating a telemedicine link with Johns Hopkins Hospital in Baltimore, MD. They are: the La Red Health Center in Georgetown, DE (this link was activated on July 10, 2013); the Peninsula Regional Medical Center in Salisbury, MD; Nanticoke Hospital In Seaford, DE; Atlantic General Hospital in Berlin, MD; Beebe Medical Center in Lewes, DE, and the Nurse-managed Health Center at the Univ. of DE. Additional Delmarvabased medical centers will probably also participate. This action will not cost the Support Group any money but is a key component of our vision as this telemedicine connection to the doctor may be the only way a person with Parkinson?s, who is living on Delmarva, is able to see a neurologist who specializes in Parkinson?s. Dr. Ray Dorsey, who started the Johns Hopkins Telemedicine initiative moved to Rochester, NY in July, 2013 and is continuing his telemedicine efforts at his new location. A MOU between the La Red Health Center and the University of Rochester Medical Center is nearing completion as the time of this writing, and after signing, Dr. Dorsey will again be able to continue to see our members via a telelink. Especially noteworthy is that Dr. Dorsey has offered to see anyone in Delaware with Parkinson?s in the convenience of their own home at no cost via a telelink.
Therapy and Exercise
This will be the most costly part of our vision to realize. Currently there are very few therapists on Delmarva trained in Parkinson-specific therapies and no trained exercise class leaders. We recently expended significant funds to get therapists and exercise class leaders from all over Delmarva trained in the latest techniques. We brought one of the leading Parkinson therapists in the nation, Dr. Becky G. Farley, founder of Parkinson?s Wellness Recovery (PWR!), to Delaware on October 26 through 29, 2013 to teach 35 therapists and 25 exercise class leaders her PWR!Clinician and Fitness classes. That program was a huge success and at least three, probably five organizations in the Rehoboth Beach/Lewes area are in the process of starting buy generic effexor xr online Parkinson?s exercise classes at the time of this writing.
Counseling
We?re expecting that a person?s medical coverage (medicare, medicaid, private insurance, other) will pick up most or all of the cost for counseling for depression and anxiety in people with Parkinson?s. Thus we don?t see counseling as a cost factor for the Support Group. We are working to develop a Mental Health capability for our members that has a number of features:
1. We are trying to start small regional support sub-groups where 6 to 12 members meet to provide mutual support to each other. Our main group has 200 members and we aren’t good at supporting each other very well, mainly because of our size.
2. We are starting small Parkinson Wellness Recovery (PWR) exercise classes in the same regional areas which will give the local members another opportunity to get to know each other better (and support each other better.)
3. We are working with social workers/guidance counselors to show us how to how to discuss Parkinson patient and caregiver needs and better support each other in various ways.
4. We are meeting socially to develop closer friendships and enjoy each others company.
We are also trying to develop a telepsychiatry capability for our members. Whole-patient oversight by a nurse The Affordable Care Act emphasizes both Wellness and the need to do a better job managing chronic conditions to include Parkinson?s. We plan to find a nurse who can work with our members on a one-to-one basis to optimize the medical, therapy and exercise, and mental health care the individual is receiving We are working with local medical centers to absorb the cost of this effort, or possibly find retired nurses to perform this function on a voluntary basis.
Summary
Not too many years ago, medical treatment of Parkinson?s was pretty much limited to medical treatment by doctors and that was largely restricted to adjusting a patients medications. For many of our members that is still the extent of medical treatment they receive today. We are trying to expand the local medical treatment capability. We are also improving our members quality of life by other means including getting therapists trained in the right kind of therapy and following the therapy with similar exercise programs. There are extensive studies showing that exercise is the only thing that affects the course of the disease. It slows the progression of Parkinson?s. With certain patients exercise may be equally or more important than medicine. The National Parkinson Foundation 2012 “Parkinson?s Outcomes Project” said that depression was the #1 factor affecting the quality of life for people with Parkinson?s. Any attempt to treat people with Parkinson?s must include a program to address their mental health, and we are attempting to do that with the various initiatives described above. In summary, we are planning to find someone who can look at the whole person, what they?re doing about their Parkinson?s, what they?re doing about any other medical conditions they have, and recommending a future course of action that will have an optimum impact on their quality of life.
